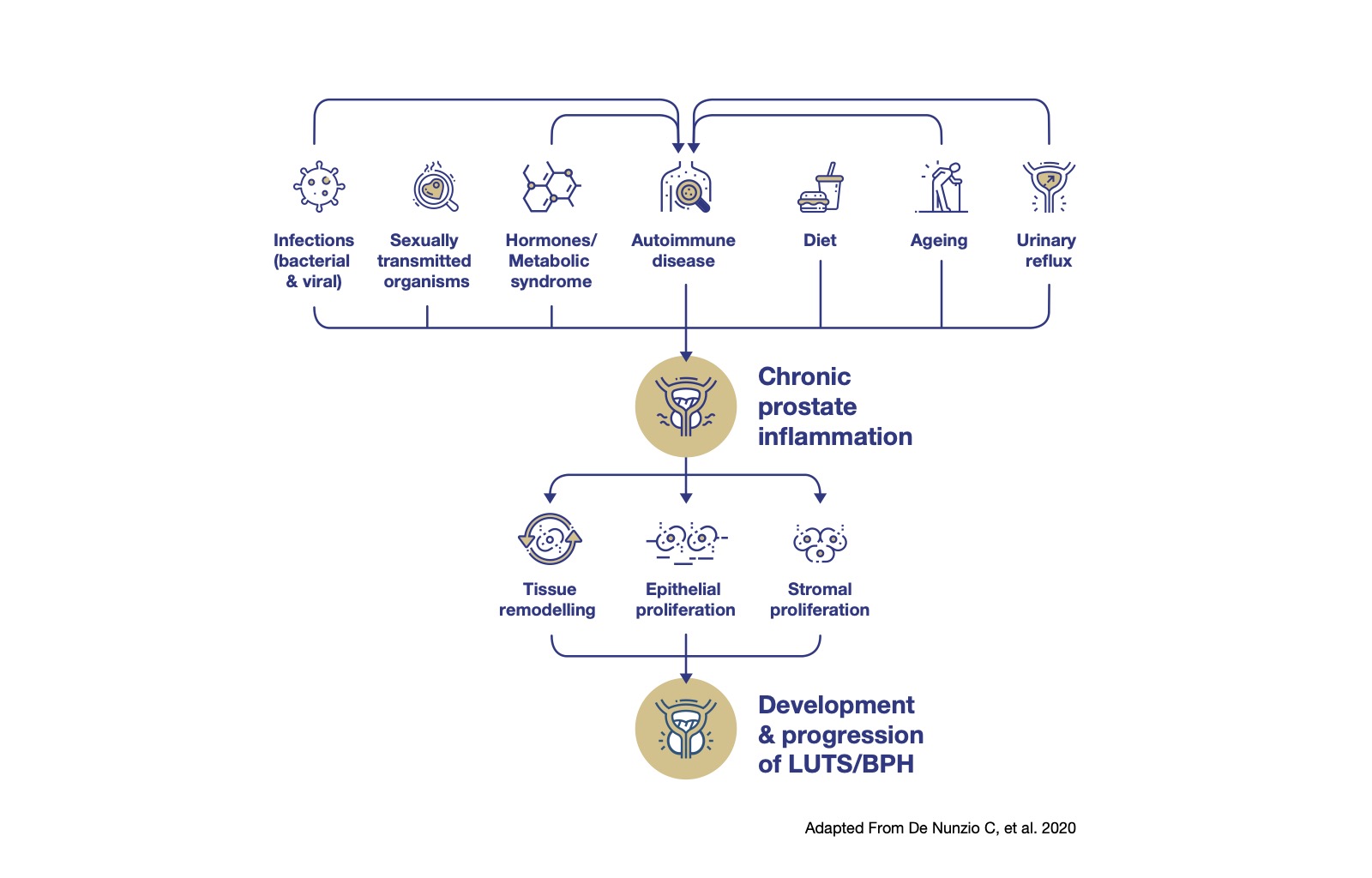
Persistent prostatic inflammation status is associated with both the development and progression of lower urinary tract symptoms (LUTS) / benign prostatic hyperplasia (BPH).1
Prostatic inflammation and development of BPH1
Chronic prostate inflammation (CPI) is identified as an important etiological component in the development of BPH. A chronic prostate inflammation is characterized by inflammatory cell infiltration within the prostatic tissue, predominantly consisting of T lymphocytes, as well as B lymphocytes and macrophages. These activated immune cells release pro-inflammatory cytokines, inducing the expression of several growth factors resulting in abnormal proliferation of epithelial and stromal prostate cells. The subsequent increased oxygen demand of these cells leads to local hypoxia producing low levels of reactive oxygen species (ROS) promoting angiogenesis and the production of additional growth factors.